Researchers found a way to direct stem cells by magnets
 Collaboration between researchers at Emory University and Georgia Institute of Technology (Georgia Tech) resulted in the development of stem cells that can be directed by magnetic fields. Stem cells could soon be intravenous injected into the patient to treat heart diseases and vascular problems. By loading stem cells with superparamagnetic iron oxide nanoparticles (SPIOs), scientists can then use magnets to deliver them to areas of the injury or disease.
Collaboration between researchers at Emory University and Georgia Institute of Technology (Georgia Tech) resulted in the development of stem cells that can be directed by magnetic fields. Stem cells could soon be intravenous injected into the patient to treat heart diseases and vascular problems. By loading stem cells with superparamagnetic iron oxide nanoparticles (SPIOs), scientists can then use magnets to deliver them to areas of the injury or disease.
The research team used human mesenchymal stem cells (hMSCs) that can be easily derived from adult tissues such as bone marrow or fat. This type of stem cells can differentiate into a variety of cell types including: bone, fat and cartilage cells, but not other types of cell such as muscle or brain. HMSCs secrete factors that inhibit inflammatory processes as well as nourishing factors, which make them promising cell population for treating conditions such as cardiovascular disease or autoimmune disorders.
Nanoparticles of magnetized iron oxide are already FDA-approved for diagnostic purposes with magnetic resonance imaging. Similar particles were used for loading stem cells in the previous studies, but coating on the particles was either toxic or changed the cells’ properties.
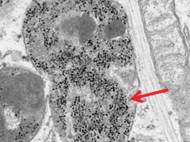
The research team used SPIOs coated with the non-toxic polymer polyethylene glycol that protects the cell from damage. The particles have an iron oxide core that is about 15 nanometers across. Furthermore, researchers used a magnetic field to push polyethylene glycol-coated SPIOs into the cells, rather than previously used chemical agents.
“We were able to load the cells with a lot of these nanoparticles and we showed clearly that the cells were not harmed. The coating is unique and thus there was no change in viability and perhaps even more importantly, we didn’t see any change in the characteristics of the stem cells, such as their capacity to differentiate”, said Robert Taylor, professor of medicine and biomedical engineering and director of the Division of Cardiology at Emory University School of Medicine.
SPIOs appear to be localized primarily in secondary lysosomes of hMSCs, which are parts of the cell that break down waste. The researchers claim that there is no degradation of the material withing the first week, because they haven’t detected any leakage of iron particles. The scientists measured the iron content in the cells once they were loaded up and determined that each cell absorbed roughly 1.5 million particles.
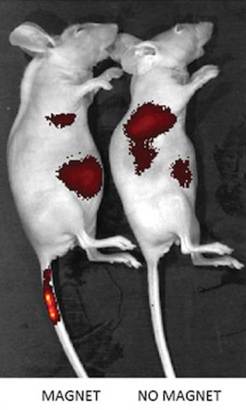
The Emory/Georgia Tech team tested the ability of magnets to steer SPIO-containing cells both in cell culture and in mice. They labeled the cells with a fluorescent dye in order to track where the cells went inside the mice. During injection of these cells into the mice’s body, a bar magnet was applied to the part of the tail close to the body and it attracted injected stem cells to the tail.
Normally most of the mesenchymal stem cells would become deposited in the lungs or the liver. The bar magnet made hMSCs loaded with SPIOs six times more abundant in the tail. Additionally, the iron oxide particles themselves could potentially be used to follow cells’ progress through the body.
The use of magnetic stem cells could have a broad spectrum of applications in medicine. Eventually, scientists could target these cells to a particular limb, an abnormal blood vessel or even the heart.
“Next, we plan to focus on therapeutic applications in animal models where we will use magnets to direct these cells to the precise site need to affect repair and regeneration of new blood vessels”, said Taylor.
For more information, read the article published in Small: “Magnetic Targeting of Human Mesenchymal Stem Cells with Internalized Superparamagnetic Iron Oxide Nanoparticles“.









Leave your response!